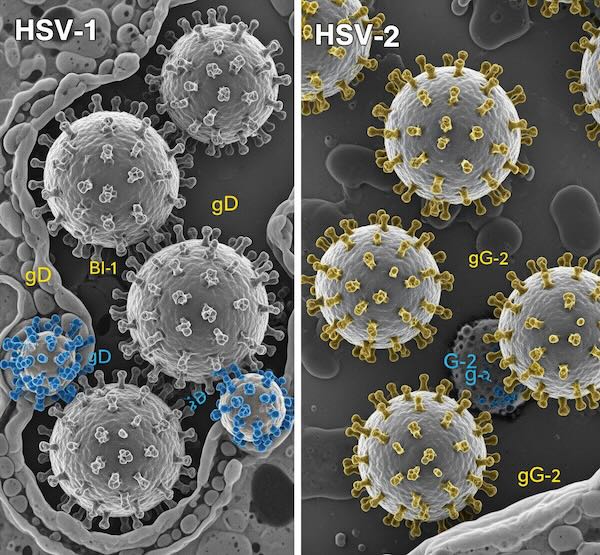
Genital HSV-1 vs. Genital HSV-2: What’s the Real Difference?
There are two types of the herpes simplex virus: HSV-1 and HSV-2.
Think of them as cousins, not identical twins.
Historically, HSV-1 was known as oral herpes (cold sores).
And HSV-2 was known as genital herpes.
But here’s the game-changer: oral sex has mixed everything up.
Now, it’s super common to get HSV-1 genitally.
And you can, though it’s less common, get HSV-2 orally.
The location of the infection doesn’t change the virus type.
So what’s the actual, practical difference for you?
It really comes down to one thing: how often it comes back.
- Genital HSV-2: This one is more at home in the genital region. It tends to cause more frequent recurrent outbreaks. We’re talking an average of 4-5 times in the first year.
- Genital HSV-1: This one is less comfortable in the genital area. After the first outbreak, it often causes very few recurrences. Many people with genital HSV-1 have maybe one more outbreak in their entire life, or none at all.
That’s the main difference you’ll likely experience.
How Do You Get Them? The Transmission Lowdown
It’s simple.
Skin-to-skin contact with the infected area.
This can be through vaginal, anal, or oral sex.
The biggest misconception is that you can only spread it when you have a sore.
Wrong.
The virus can “shed” from the skin even when there are no symptoms.
This is called asymptomatic shedding.
This is actually how most people get it.
Someone who doesn’t even know they have it passes it on.
- Genital HSV-1 is most often transmitted from someone with an oral cold sore (HSV-1) to a partner’s genitals during oral sex.
- Genital HSV-2 is most often transmitted through genital-to-genital contact.
Condoms help, a lot. But they aren’t 100% foolproof because they don’t cover all the skin.
Want to know more? Learn more about Herpes Testing.
Risks and Complications: What You Need to Know
For most healthy people, genital herpes is not medically dangerous.
It’s an annoying skin condition. That’s it.
The biggest complication for most is the psychological impact.
The stigma, the shame, the fear of telling partners. That’s the real heavy lifting.
Physically, the risks are very low.
In extremely rare cases, especially in people with severely weakened immune systems, the infection can spread and cause more serious issues.
But for the average person? The main risk is passing it to a sexual partner.
Treatment and Management: Taking Control
You can’t cure it. Let’s get that out of the way.
But you can manage it so well that it has a minimal impact on your life.
Your main tool is antiviral medication.
You have two ways to use it:
- Episodic Therapy: You take pills for a few days as soon as you feel an outbreak coming on (tingling, itching). This makes the outbreak shorter and less severe.
- Suppressive Therapy: You take a low-dose pill every single day. This is a game-changer. It can reduce the number of outbreaks you have by 70-80% and, crucially, cut the risk of transmission to a partner by about 50%.
It’s about deciding what works for you. If you have infrequent outbreaks (common with genital HSV-1), you might just treat them as they come. If they’re frequent and bugging you (more common with HSV-2), daily therapy might be your best bet.
Ready to take the next step? Learn More on Testing and Treatment of Genital Herpes
Pregnancy and Herpes: A Special Consideration
This is where you need to be proactive.
If you have genital herpes and you’re pregnant, you must tell your doctor.
The main concern is passing the virus to the baby during birth, which is called neonatal herpes.
Neonatal herpes is rare, but it is very serious.
Here’s the deal:
- The risk is highest if you get your first-ever herpes outbreak late in your third trimester. Your body hasn’t had time to create antibodies to pass to the baby.
- The risk is very low if you had herpes before you got pregnant. Your body has antibodies, and you pass them to the baby, giving them protection.
So, what do doctors do?
To be safe, they’ll likely put you on daily suppressive antiviral therapy from about 36 weeks of pregnancy until you deliver.
This massively reduces the chance of you having an outbreak when you go into labour.
If you have active sores or symptoms of an outbreak when it’s time to deliver, your doctor will recommend a Caesarean section to prevent the baby from coming into contact with the virus in the birth canal.
It’s all about communication with your healthcare team.
FAQs
1. Can I still have a normal sex life? Absolutely. It’s about communication, using protection, and possibly using suppressive therapy to lower the risk to your partner.
2. How do I know which type I have? You need a specific blood test (a type-specific IgG test) or a swab test taken directly from a sore. The swab is the most accurate way.
3. Can you get rid of herpes forever? No. It’s a virus that lives in your nerve cells for life. But you can manage the symptoms.
4. Is one type “better” to have than the other genitally? If you had to choose, genital HSV-1 is generally considered “better” simply because it causes far fewer outbreaks after the first year.
5. What do outbreaks feel like? It starts with a tingling, itching, or burning sensation. Then, one or more blisters appear, which break and turn into shallow sores. They then scab over and heal in about 1-2 weeks.
6. How effective is suppressive therapy? Very. It can reduce outbreaks by 70-80% and cut the transmission risk by about half. Thinking about your options? Explore daily suppressive therapy options in detail.
7. Can condoms prevent transmission completely? No. They reduce the risk significantly but don’t eliminate it because the virus can be on skin that the condom doesn’t cover.
8. What should I do if I think I have herpes? See a Dermatologist or Come visit our Derma clinic as soon as you have symptoms. Getting tested is the best way to get a definite diagnosis.
Understanding the facts about Genital HSV1 vs Genital HSV2 is your first and most powerful tool for taking control of your health. For HSV 1 and HSV 2 testing, treatment and consultation please visit Derma Clinic Kathmandu. Contact us via whatsapp or call at 9801358600